From UC San DiegoReviewed by Dan Hutchins, M.PhilJun 11 2021
By observing what was going on across the world in early 2020, researchers from the University of California San Diego School of Medicine knew that their region would soon be flooded with patients infected with COVID-19—the disease caused by SARS-CoV-2.
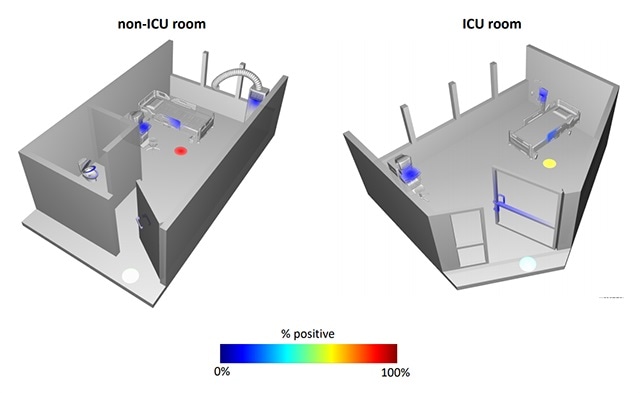
This schematic shows some of the locations where SARS-CoV-2’s genetic signature was detected in the intensive care unit (ICU) and other hospital rooms. Image Credit: University of California San Diego.
The researchers were curious to know how the virus survived on surfaces, particularly in hospitals, and they knew they only had a little time to get started if they wanted to take a snapshot of the “before” condition, that is, before people with the infection were hospitalized.
After receiving a call late one Sunday night, a crew gathered the next day in the hospital lobby, ready to swab. In the ensuing study, the researchers swabbed the surfaces of patient rooms before, during, and after occupancy, and collected samples from the noses, stool, and skin of COVID-19 patients and their health care staff over time. The study was published in the Microbiome journal.
Over the course of two months, the team tested as many as 972 hospital-associated samples for SARS-CoV-2 evidence.
Although it feels like we’ve been living with this virus for a long time, the study of the interactions between SARS-CoV-2 and other microbes is still new, and we still have a lot of questions. The more we know about how a virus interacts with its environment, the better we can understand how it’s transmitted and how we might best disrupt transmission to prevent and treat the disease.”
Sarah Allard, PhD, Study Co-Senior Author and Assistant Project Scientist, UC San Diego School of Medicine and Scripps Institution of Oceanography
The team’s study results: The virus, or at least its genetic signature, is everywhere. The virus was found on flooring near the beds of COVID-19 patients (39% of samples tested), flooring outside the patient rooms (29%), and surfaces within the rooms (16%). The detection of SARS-CoV-2 was the highest in the first five days after the onset of symptoms.
But the researchers quickly pointed out that just because they can identify the unique genetic signatures of the virus on a surface does not imply that the virus can infect individuals. Since the study’s inception, it has been widely demonstrated that SARS-CoV-2 transmits predominantly via close human encounters, with surface transmission being extremely unlikely.
Furthermore, none of the study’s health care staff, who were actively caring for patients, had tested positive for the virus. The study only looked at one hospital, but the researchers believe that similar results would be seen in any hospital that is treating COVID-19 patients.
This is huge on so many levels. We need to know if our personal protective equipment, PPE, is adequate, and fortunately we know now that things like masks, gloves, gowns and face shields really do work. This pandemic has been a global disaster, but it could’ve been even worse if our health care workers were getting infected, especially if we didn’t know why.”
Daniel Sweeney, MD, Study Co-Senior Author and Critical Care and Infectious Disease Physician, UC San Diego Health
Viruses do not usually hang out by themselves. Whether on individuals or surfaces, these pathogens are part of complex communities called microbiomes, which may comprise a range of different bacteria, viruses, and additional microorganisms.
While searching for the coronavirus, the researchers noticed something else: a specific form of a bacterium, from the genus Rothia, was often detected alongside SARS-CoV-2, independent of the site of collection. This means, the presence of Rothia strongly indicated that they would also identify the SARS-CoV-2 in the same sample.
Why that relationship? Do the bacteria help the virus survive, or vice versa? Or is it just that these bacteria are associated with the underlying medical conditions that put patients at higher risk for severe COVID-19 in the first place? That’s an area for future research.”
Sarah Allard, PhD, Study Co-Senior Author and Assistant Project Scientist, UC San Diego School of Medicine and Scripps Institution of Oceanography
The research was tough from the start, and it grew more challenging when the hospital’s critical care unit began to admit more COVID-19 patients. The team specifically developed their method to harness the existing resources to avoid straining the supply chain required for clinical treatment and testing.
Some members of the team and their collaborators created alternate swabs for research purposes in a separate initiative. They gathered samples as rapidly and as effectively as possible to cause minimal disturbance to patient care. The samples were returned to the laboratory in alcohol, which preserved the virus for more analysis without exposing the researchers to active organisms.
“A lot of people did a lot of basic and clinical research these last few months, and we did it well. We added to our infrastructure. We acquired the experience. I hope the same sort of focus, drive and spirit carry forward in whatever comes next,” concluded Sweeney.
Source:
Journal reference:
Marotz, C., et al. (2021) SARS-CoV-2 detection status associates with bacterial community composition in patients and the hospital environment. Microbiome. doi.org/10.1186/s40168-021-01083-0.