Passive immunity to diseases can be developed through the transfer of antibodies. This occurs naturally in infants, from the mother to the child in pregnancy or while breastfeeding, and reduces the risk of the child getting diseases while developing the adaptive immune system.
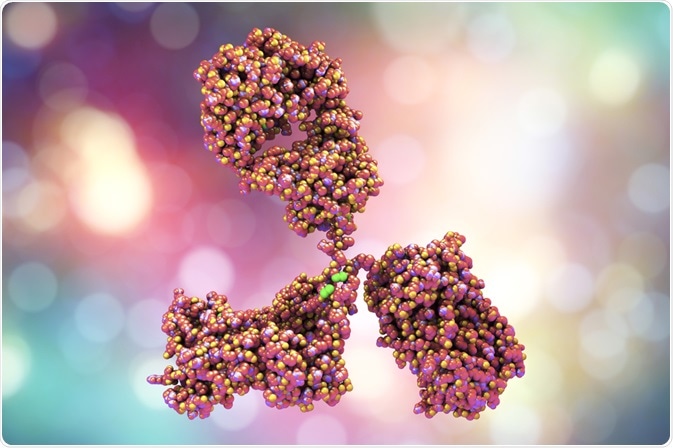
Image Credit: Kateryna Kon/Shutterstock.com
Artificially-gained passive immunity can be achieved through various mechanisms, including the injection of monoclonal antibodies (mAbs). This only provides the recipient with temporary immunity, as the antibodies eventually degrade.
This approach is often used to treat certain cancers and autoimmune diseases. The Fab region of the antibody binds to receptors on the affected cell, and the Fc region attracts immune cells, toxins, or cytokines involved in the immune response.
While more common in autoimmune diseases, mAbs have also been used in anti-viral medications to target the immune system towards cells presenting viral antigens, killing infected cells before the virus can reproduce.
MB66 development
MB66 is a film that was developed by Mapp Biopharmaceutical, a pharmaceutical company dedicated to developing new drugs to meet unmet needs in the prevention and treatment of infectious diseases.
Mapp Biopharmaceutical is previously known for helping to develop ZMapp, an experimental antibody-based pharmaceutical used to treat Ebola. However, after a clinical trial during an outbreak around Kivu (east Congo), ZMapp was proven to be less effective than other available Ebola treatments.
The MB66 film should be applied to the vagina, where it releases antiviral antibodies against HIV and genital herpes (HSV). Further improvements in the technology will focus on the addition of anti-sperm cell antibodies to prevent pregnancy.
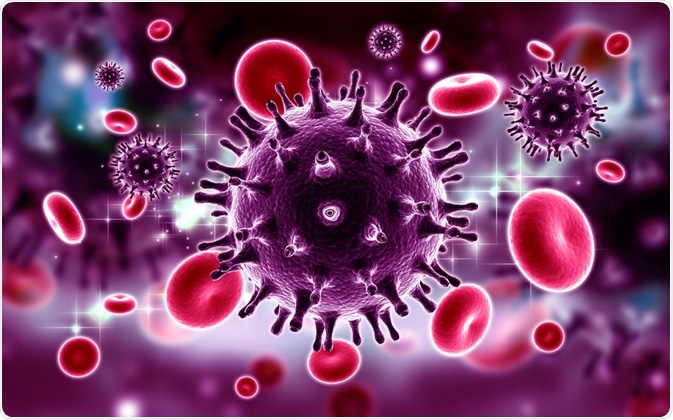
Image Credit: Raj Creationzs/Shutterstock.com
The idea is that MB66 could be seen as a more socially acceptable contraceptive than condoms, while also increasing efficacy. A widespread uptake may help to reduce the spread of HIV/HSV within the context of the global pandemic.
A study of heterosexual HIV transmission among young sub-Saharan Africans, showed non-use of condoms to be four times more likely than using them. In the long-term MB66 is a potential strategy to increase the uptake of preventative contraception in high-burden countries.
Furthermore, it would provide another alternative to current hormonal contraceptives. Many women observe significant side effects and, in the future, MB66 may provide an improvement in the quality of life for some women in both developed and developing countries.
There is also the potential for the technology to be mass-produced using plants. This would provide a potentially cheaper alternative to current methods of mAbs production. Similar experimental methods have been successful in the production of anti-rabies antibodies.
Phase 1a Clinical Trial
A phase 1a clinical trial was completed in the United States in 2018 as a collaboration between Mapp Biopharmaceutical and Boston University. The aim was to determine the safety and pharmacokinetics of MB66 in a small, single-center trial in 38 women.
Segment A involved providing 8 women with a single dose of MB66 film to determine any side effects of the technology. It had previously been shown to be safe in a rabbit model at a significantly higher dose.
After the safety of MB66 was determined, segment B was started. Participants were allocated 1:1 into groups where they received a daily dose of the MB66 film or a placebo film for 7 days. This allowed the safety of MB66 to be determined over a longer period.
Pharmacokinetic tests were also undertaken during segment B. This involved studying the rate of MB66 film dissolution, vaginal concentrations of MB66 antibodies, and the anti-HIV/HSV effect of MB66 ex vivo.
The trial also investigated the use of plants, particularly those of the genus Nicotiana (i.e. tobacco plants), to produce MB66 antibodies. This could potentially provide an efficient alternative to current production methods and, in the long-term, allow MB66 to be widely and cheaply available on the market.
Future developments
The Boston University-led consortium will lead to contraceptive developments within the product. Antibodies against sperm cells can be isolated from infertility patients and produced through monoclonal antibody technology.
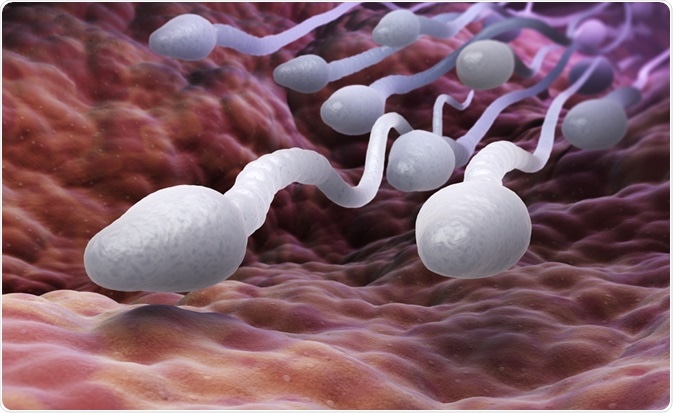
Image Credit: Tatiana Shepeleva/Shutterstock.com
There are plans to test the safety of a human contraceptive antibody (HCA) with anti-sperm cell capabilities in the phase 1 clinical trial. HCA will be tested by itself on a vaginal film, with the long-term aim of incorporating it into an MB66 film if trials are successful.
There are also plans within the consortium to use fungi to produce antibodies. As stated by Kevin J. Whaley of Mapp Biopharmaceutical, “We look forward to evaluating Trichoderma-manufactured antibodies that could meet demands of large, cost-sensitive markets.”
This method of contraception that prevents pregnancy while also including anti-viral antibodies to prevent sexually transmitted infections (STIs), could be the gold standard within the field. MB66 could potentially have a role in fighting the HIV pandemic, reducing the prevalence of HSV, and providing an alternative to condoms and hormonal contraceptives.
References
- clinicaltrials.gov (2018) Vaginal Antibody Safety Trial: Safety Study of Monoclonal Antibodies to Reduce the Vaginal Transmission of Herpes Simplex Virus (HSV) and Human Immunodeficiency Virus (HIV) - Full-Text View - ClinicalTrials.gov. Available at: https://www.clinicaltrials.gov/ct2/show/NCT02579083?term=mb66&draw=2&rank=1 (Accessed: 11 March 2020).
- mappbio.com (2018) MB66 FAQ - Mapp Biopharmaceutical, Inc. Mapp Biopharmaceutical, Inc. Available at: https://mappbio.com/ (Accessed: 10 March 2020).
- mappbio.com (2020) Antibody-based Contraceptive Research Center Awarded to Boston University Led Consortium - Mapp Biopharmaceutical, Inc. Mapp Biopharmaceutical, Inc. Available at: https://mappbio.com/ (Accessed: 15 March 2020).
- Mulangu, S. et al. (2019) ‘A randomized, controlled trial of Ebola virus disease therapeutics’, New England Journal of Medicine. Massachusetts Medical Society, 381(24), pp. 2293–2303. doi: 10.1056/NEJMoa1910993.
- Winskell, K. et al. (2020) ‘Social representations of the prevention of heterosexual transmission of HIV among young Africans from five countries, 1997-2014’, PLOS ONE. Edited by J. A. Bauermeister. Public Library of Science, 15(3), p. e0227878. doi: 10.1371/journal.pone.0227878.
Further Reading
Last Updated: Dec 29, 2022