Neutrophils are the most common type of white blood cell in the body, and an important part of the innate immune system. They were identified first by Paul Ehrlich in 1880 and were observed to phagocytosize foreign matter in 1883 by Elie Metchnikoff.
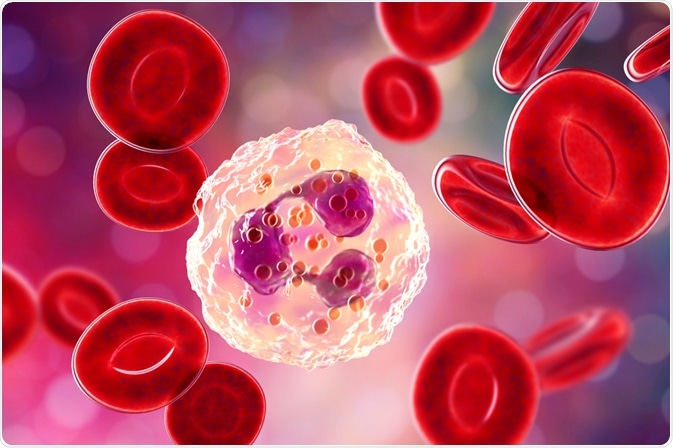
Image Credit: Kateryna Kon/Shutterstock.com
The two main functions of neutrophils in healthy individuals (i.e. non-cancerous) are in phagocytosis to prevent infection and promoting inflammation. However, they can have various additional roles, which sometimes appear to conflict, particularly in their interactions with cancer cells.
Neutrophils are smaller than macrophages, so generally phagocytosize smaller objects including foreign matter, viruses, and small bacteria.
Role in health and disease
During normal infection, neutrophils are directed to the site of infection by cytokines. This process involves chemotaxis, so the cell moves along the chemical gradient from an area of low cytokine concentration to an area of high concentration.
This occurs via a process known as neutrophil rolling, the neutrophil moves along the interior of the endothelial wall of a blood vessel through cytokine binding and blood flow. Close to the site of infection, the neutrophil will transmigrate from the blood into the tissue along the cytokine gradient.
Key cytokines include component proteins, C3a and C5a, and interleukin 8. The increased production of these messengers is promoted by immune cells at the site of infection, initiating an inflammatory response.
At the infection site, the foreign matter or foreign organism is targeted for neutrophil-mediated phagocytosis. One process by which this occurs is through the binding of antibodies to the target, the neutrophil binds Fcγ receptors on the antibody.
The foreign material is absorbed by the neutrophil by endocytosis to form a phagosome. Vesicles can then fuse with the phagosome, releasing molecules that kill and degrade the matter within. Spent neutrophils become apoptotic after this process is repeated multiple times.
After the infection, spent neutrophils display apoptotic signals, targeting them for phagocytosis by macrophages. Increasing evidence is suggesting that during the downregulation of inflammation many unutilized neutrophils can migrate back into blood vessels after infection, however, the mechanism involved is still relatively unclear.
Recently, it has also been shown that neutrophils have an additional role in the immune response containing the infective agent at the site of infection through neutrophil extracellular traps.
Neutrophils release granule proteins and chromatins, this forms an extracellular matrix that prevents foreign material from the site of infection. This may be key in preventing the evasion of the immune system and to help other immune cells identify and act upon the infection, stimulating a local inflammatory response.
Image Credit: SciePro/Shutterstock.com
Role in the context of cancer
There are conflicting reports and much debate about the function of neutrophils in the context of cancer and their contribution to disease progression and tumor growth. This has led to a discussion on the previously through homogeneity of neutrophils in the body.
Different studies have shown neutrophils to release tumor-promoting cytokines, support metastasis of tumor cells, and promote angiogenesis within tumors. However, other studies have demonstrated neutrophils to stimulate the anti-tumor immune response and inhibit tumor growth and metastasis by cytotoxic mechanisms.
This indicates the presence of neutrophil sub-populations, and the phenomenon has also been observed to a lower extent in other diseases such as HIV infection, psoriasis, and malaria.
One proposed marker of breaking neutrophils into subsets is by their physical properties, particularly density. Higher density neutrophils (HDNs) migrate in a granulocytic fashion along with other HDNS, whereas lower density neutrophils (LDNs) migrate in a monocellular fashion.
However, a problem with this is that neutrophils are highly sensitive to their environment and likely gain properties when they enter the tissue. For example, it is not clear whether neutrophils gain tumor-promoting properties when entering tumor tissue, or if they belong to a subset of naturally occurring tumor-promoting neutrophils.
It is also unclear whether neutrophils exist in sub-populations at all similar to T cells, split into T helper cells, T regulatory cells, etc. This may rather exist in a continuum of neutrophil phenotypes across a spectrum due to a high level of responsiveness to their microenvironment.
Understanding the heterogeneity of neutrophils is a developing field within immunology and further research is required to determine to subset v. continuum debate. This may be particularly relevant to understanding the role of neutrophils in the unique microenvironment of cancer.
The identification of sub-populations also raises many further questions. This includes whether different subsets are pro-inflammatory compared to others being anti-inflammatory, and the subsets affect the progression of the disease, including cancer.
The currently limited division of neutrophils based on physical properties will likely be insufficient to properly understand the complexities of neutrophil involvement in the immune response and their interactions with other cells. However, this will be seen through further research as the field evolves.
References
- Jablonska, J. and Granot, Z. (2017) ‘Neutrophil, quo vadis?’, Journal of Leukocyte Biology. Wiley, 102(3), pp. 685–688. doi: 10.1189/jlb.3mr0117-015r.
- Lee, W. L., Harrison, R. E. and Grinstein, S. (2003) ‘Phagocytosis by neutrophils’, Microbes, and Infection. Elsevier Masson SAS, 5(14), pp. 1299–1306. doi: 10.1016/j.micinf.2003.09.014.
- Liew, P. X. and Kubes, P. (2019) ‘During Health and Disease’, Physiol Rev, 99, pp. 1223–1248. doi: 10.1152/physrev.00012.
Further Reading
Last Updated: Jul 28, 2020