Immune checkpoints are proteins or protein complexes that lie at strategic points in cellular pathways involved in the regulation of the immune system. Therefore, these molecules are good targets for immunotherapy, particularly in cancer treatment.
Image Credit: Alpha Tauri 3D Graphics/Shutterstock.com
Monoclonal antibodies (mAbs) can be designed to target immune checkpoints. They can, for example, promote activation of the immune system by binding a molecule that represses the recruitment of immune cells.
This is can help lead to a reduced number of diseased target cells by promoting T cell-mediated cell death, so it is particularly useful in cancer therapy where mechanisms that normally activate the immune system or control cell growth are often downregulated.
Immune checkpoint therapy in cancer patients
Immune checkpoints are a key target of cancer immunotherapy. In cancer cells, these checkpoints can be down- or upregulated depending on their role in activating or inhibiting the immune response.
CTLA-4 is an immune checkpoint that is upregulated in many cancers. It is found in regulatory T cells, as well as T cells after activation, and is involved in inhibition of the immune response. Overexpression of this protein allows tumors to evade the immune system.
Ipilimumab was the first immune checkpoint inhibitor that was approved by the FDA. It targets CTLA-4, preventing downregulation of the immune system, while also activating helper T cells and cytotoxic T cells and recruiting them to target sites.
Another important checkpoint in the suppression of the immune response is PD-1 and its ligand PD-L1. In a normal environment, this interaction is involved in suppressing the immune response after infection occurs, preventing host cells from being targeted, and the development of autoimmune disease.
In many cancers the production of PD-L1 is upregulated, leading to overstimulation of PD-1 on regulatory immune cells. This acts to contribute to suppression of the immune response around tumor sites.
Nivolumab is an immune checkpoint inhibitor that targets PD-1 and has shown good results in some cancers. For example, in urothelial bladder cancer, the overall response rate increased from 13% to 24% compared to a control group.
Similar moderate improvements in response were observed in other cancers including Hodgkin’s lymphoma and triple-negative breast cancer.
Unfortunately, evidence indicates that very few cancer patients can benefit from such therapies, with some developing severe side effects as a result of this immune checkpoint inhibitors. This is likely due to complex interactions between the immune system and the tumor micro-environment.
Biomarkers may be able to suggest whether a patient is suitable for this therapy if it should be combined with other therapies, or avoided altogether. However, this is an area of future research to improve the predictability of the success of specific therapy in a patient.
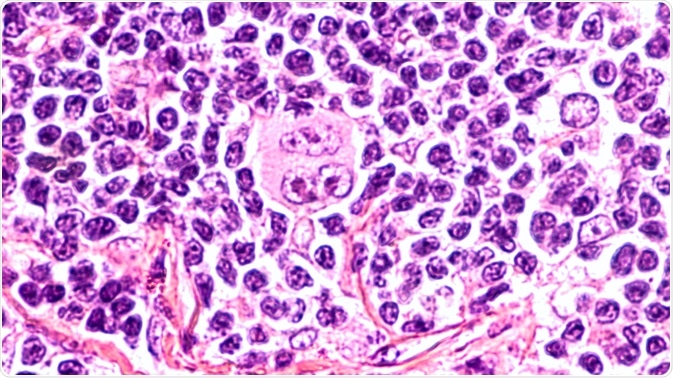
Image Credit: David A. Litman/Shutterstock.com
Other disease areas for immune checkpoint therapy
A possible approach is to target molecules on immune cells responsible for conferring signals within the cell. This could inhibit molecules involved in the repression of the immune response, leading to an increased concentration of immune cells at a target site.
For example, Siglecs are a family of cell surface proteins that bind sialic acid-containing glycans, these interactions are involved in pathways for cell signaling and cell adhesion, among others. They are uniquely found on immune cells and have been linked to negative regulation of some parts of the immune response.
Siglec-9 is found on monocytes and neutrophils, and inhibition with anti-Siglec-9 autoantibodies has been shown to have an anti-inflammatory effect. This would suggest a potential role of immune checkpoint therapy against an allergic response, or similar inflammatory diseases.
While Siglec-9 isn’t normally found on T cells, it is shown to be present on T cells that infiltrate solid tumor tissue. This could represent an area for potential therapies, as it isn’t normally found on T cells any therapy could be highly specific in the recruitment of relevant T cells to tumor sites.
Siglec-8 is found mainly on mast cells and eosinophils. Antibodies against it have been shown to induce apoptosis of these cells and in mouse models, a reduced number of eosinophils can be seen.
In patients with systemic mastocytosis, an accumulation of defunct mast cells, a mAb against Siglec-8 initiated cytotoxic T cell-mediated killing of mast cells, representing a possible therapy for this rare disease.
Anti-Siglec-8 antibodies have been suggested for bronchial asthma and were seen to be safe in a phase I clinical trial. However, research needs to be conducted in this area before this is a viable option.
Conclusion
Immune checkpoint therapy represents a new and clinically relevant avenue of immunotherapy research. Targeting checkpoints is useful in preventing immune suppression or to initiate an immune response, depending on the nature of the disease.
More research is necessary to develop therapies that a widely applicable and to understand who can benefit from these therapies. However, this area does have significant potential both in cancer and in autoimmune and inflammatory diseases
References
- Darvin, P. et al. (2018) ‘Immune checkpoint inhibitors: recent progress and potential biomarkers’, Experimental and Molecular Medicine. Nature Publishing Group. doi: 10.1038/s12276-018-0191-1.
- Li, Z. et al. (2018) ‘Recent updates in cancer immunotherapy: A comprehensive review and perspective of the 2018 China Cancer Immunotherapy Workshop in Beijing’, Journal of Hematology, and Oncology. doi: 10.1186/s13045-018-0684-3.
- Lin, C. H., Yeh, Y. C. and Yang, K. D. (2019) ‘Functions and therapeutic targets of Siglec-mediated infections, inflammations, and cancers’, Journal of the Formosan Medical Association. Elsevier B.V. doi: 10.1016/j.jfma.2019.10.019.
Further Reading
Last Updated: Jun 23, 2020