Mesenchymal stem cells, or MSCs, have the ability to differentiate into an array of different types of cells, such as fat, bone, and muscle cells.
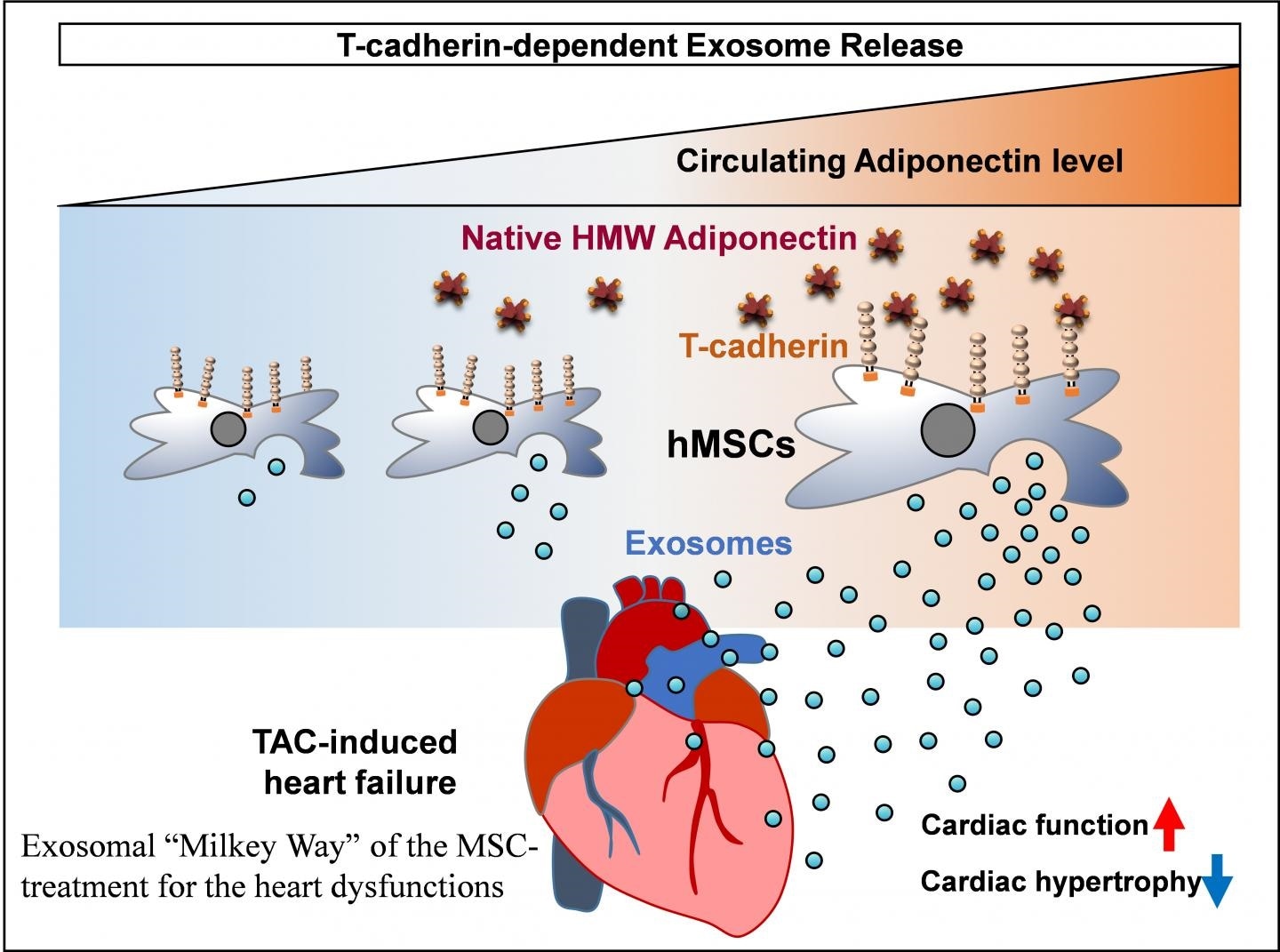
Mesenchymal stem cell (MSC) therapies are being developed for the treatment of various diseases, including heart failure and ARDS caused by COVID-19 infection. Nakamura et al. demonstrated the importance of adiponectin in circulation and the expression of T-cadherin by human adipose-derived MSCs for enhanced exosome synthesis, resulting in improved cardiac function in a heart failure model. Image Credit: Copyright© 2020 Molecular Therapy. All right reserved.
However, the ability of these cells to activate the repair of damaged tissues has attracted the interest of scientists across the world, with MSCs showing therapeutic effects in the treatment of various conditions, like liver cirrhosis, diabetes, and heart disease.
But in spite of the success of many clinical trials, scientists have strived to describe the sometimes-variable outcomes of MSC therapy.
In a new research published in the Molecular Therapy journal, a team of researchers headed by Osaka University examined the potential reasons for the variable results of MSC therapy, demonstrating that host factors may be to blame other than only the MSCs.
We recently reported that adiponectin, a beneficial hormone secreted by fat cells that plays a role in muscle regeneration, binds to receptor protein T-cadherin on cell surfaces. Given that T-cadherin is abundant on the surfaces of MSCs, we investigated whether adiponectin is involved in the regenerative activity of MSCs in a model of heart failure.”
Yuto Nakamura, Study Lead Author, Osaka University
Blood contains high concentrations of adiponectin, which has been demonstrated to trigger the production of exosomes—tiny membrane-bound vesicles that carry DNA, lipids, and proteins between cells. Fascinatingly, exosomes released by stem cells transport signals that trigger the repair of recipient cells.
The scientists initially quantified the production of exosomes in a cell culture-based system and verified that increasing concentrations of adiponectin resulted in a corresponding increase in the abundance of exosomes derived from MSCs. These exosomes depend on the expression of T-cadherin.
When MSCs were injected into mice affected by heart failure, it considerably enhanced the cardiac function of the left ventricle, which was related to the increased number of circulating exosomes. Most significantly, cardiac function after MSC therapy could be additionally reinforced by the increased levels of adiponectin in blood.
Together, our assays showed that MSCs exert their therapeutic effects on cardiac function through the production of exosomes, which is influenced by host plasma adiponectin levels and is reliant on MSC T-cadherin expression.”
Shunbun Kita, Study Corresponding Author, Osaka University
Kita continued, “Given these results, drugs such as PPARγ agonists, which increase adiponectin production, could be administered in combination with MSC therapy to significantly enhance the therapeutic potential—not only for severe heart failure, but also for a variety of diseases involving tissue damage, including COVID-19-associated acute respiratory distress syndrome.”
And if one is speculating, it turns out that excess fat is truly detrimental to the production of adiponectin, which means physicians will not be prescribing a high fat diet in the near future.
Source:
Journal reference:
Nakamura, Y., et al. (2020) Adiponectin Stimulates Exosome Release to Enhance Mesenchymal Stem-Cell-Driven Therapy of Heart Failure in Mice. Molecular Therapy. doi.org/10.1016/j.ymthe.2020.06.026.