A new study published recently in the eLife journal shows that the bacterial equivalent of a traffic jam leads to the formation of multilayered biofilms in the presence of antibiotics.
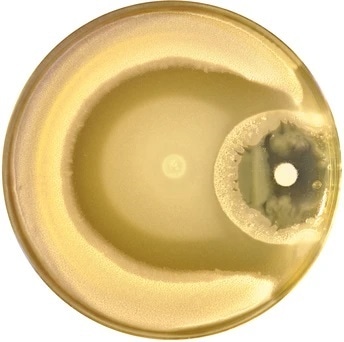
Swarming Bacillus subtilis cells form a multilayered biofilm in a dish when exposed to the antibiotic kanamycin (pictured here on the right-hand side of the dish). Image credit: Grobas et al.
The study demonstrates the way in which the collective behavior of bacterial colonies may lead to antibiotic resistance. This understanding could open the door to new methods for treating bacterial infections that help inhibit the emergence of antibiotic resistance.
Genetic mutations cause bacteria to acquire antibiotic resistance. However, they can also safeguard themselves through collective behaviors like swarming together in a biofilm—a thin, slimy film composed of several bacteria that is less vulnerable to antibiotics.
Moreover, swarms of bacteria can sustain a phenomenon analogous to human traffic jams known as “motility-induced phase separation,” where they slow down when large numbers of bacteria cram together.
In our study, we wanted to see whether swarming bacteria can use physical interactions such as motility-induced phase separation to overcome certain stresses including exposure to antibiotics.”
Iago Grobas, Study First Author and PhD Student, Warwick Medical School, University of Warwick
As part of the study, a swarm of a common environmental bacteria called Bacillus subtilis was exposed by Grobas and his team to an antibiotic known as kanamycin in a dish in the lab. A time-lapse video of the bacteria’s behavior was recorded, and it was discovered that they developed biofilms when the drug is present.
The researchers mainly demonstrated that the biofilm develops since bacteria start grouping together a distance away from the antibiotic, which makes way to several layers of swarming bacteria.
The layers build up through a physical mechanism whereby groups of cells moving together collide with each other. The collision generates enough stress to pile up the cells, which then move slower, attracting more cells through a mechanism similar to motility-induced phase separation. These multiple layers then lead to biofilm formation.”
Iago Grobas, Study First Author and PhD Student, Warwick Medical School, University of Warwick
Then, the researchers tested an approach to inhibit this formation and thus suppress antibiotic resistance from emerging in this way. It was discovered that when a single dose was split in two steps without altering the total amount of antibiotics, the emergence of a biofilm was strongly inhibited.
According to the researchers, more studies are now required to identify whether bacteria dangerous to humans use analogous behaviors to survive exposure to antibiotics. If they do survive, then future treatments should consider these behaviors to reduce antibiotic resistance.
Our discoveries question the way we use antibiotics and show that increasing the dosage is not always the best way to stop biofilm development. The timing of the bacteria’s exposure to drugs is also important.”
Munehiro Asally, Study Co-Senior Author and Associate Professor, School of Life Sciences, University of Warwick
“These insights could lead us to rethink the way antibiotics are administered to patients during some infections,” concluded Marco Polin, co-senior author of the study, Associate Professor at the Department of Physics, University of Warwick, and a researcher at the Mediterranean Institute for Advanced Studies (IMEDEA), Mallorca.
Source:
Journal reference:
Grobas, I., et al. (2020) Swarming bacteria undergo localized dynamic phase transition to form stress-induced biofilms. eLife. doi.org/10.7554/eLife.62632.