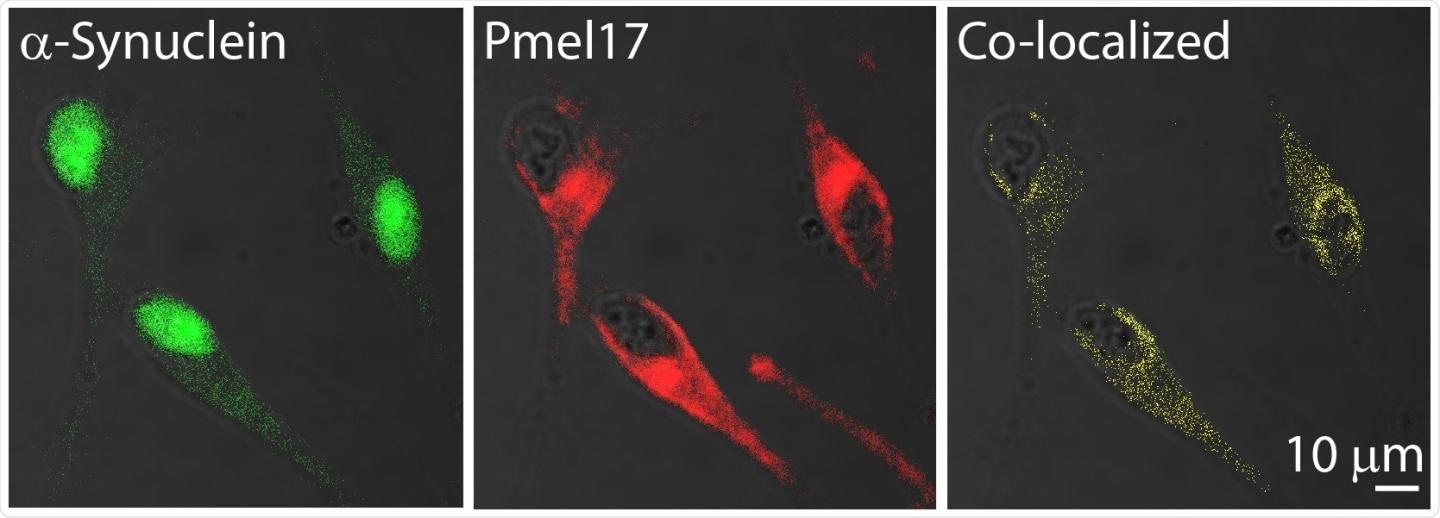
Immunofluorescence images show that some α-synuclein and Pmel17 are in the same locations in human melanoma cells. Image Credit: Dexter Dean, PhD.
However, for almost five decades, physicians have recognized that patients with Parkinson’s disease have a higher risk of developing melanoma when compared to the general population. And researchers have now reported a molecular connection between these two disorders in the form of protein aggregates, called amyloids.
The team will present their findings at ACS Spring 2021—the spring meeting of the American Chemical Society (ACS)—which is being conducted online from April 5th to 30th, 2021.
During the meeting, live sessions will be hosted from April 5th to 16th, 2021, and networking and on-demand content will go on through April 30th, 2021. The meeting includes almost 9,000 presentations on a broad range of science topics.
Several studies have shown that melanoma occurs two to six times more frequently in the Parkinson's population than the healthy population. What’s more, the protein involved in Parkinson’s disease, α-synuclein, is elevated in melanoma cells.”
Dexter Dean, PhD, Postdoctoral Fellow, National Heart, Lung, and Blood Institute
Dean is presenting the study at the ACS meeting.
α-synuclein creates amyloid deposits in Parkinson’s disease and these deposits are believed to destroy dopamine-releasing neurons in the brain, inducing many symptoms, like tremor, dementia, and slow movements. Although active research works have targeted the impacts of α-synuclein in the brain, not much is known about its activities or presence in other tissues.
But investigators have proof that there is more expression of an amyloid-forming protein in melanoma cells when compared to that in healthy skin.
Besides this, increased concentrations of α-synuclein in melanocytes (the skin cells that cause melanoma) correspond with reduced production of pigment, or melanin. This pigment prevents damage caused to the skin by the sun’s ultraviolet rays.
Jennifer Lee, Ph.D., Dean’s postdoctoral advisor at National Heart, Lung, and Blood Institute (NHLBI), which is part of the National Institutes of Health, has already investigated premelanosomal protein (Pmel), which is another amyloid-forming protein.
Most people know that amyloids are involved in diseases, such as Parkinson's and Alzheimer's, but it's less well-known that some amyloids, like Pmel, actually serve a useful function.”
Jennifer Lee, PhD, Postdoctoral Advisor, National Heart, Lung, and Blood Institute
Pmel forms amyloid fibrils in healthy melanocytes. These fibrils serve as scaffolds to preserve melanin in melanosomes—the organelle in which the pigment is created, preserved, and transported.
“Because both α-synuclein and Pmel are expressed in melanoma cells, we wondered if these two amyloid proteins could interact and whether this interaction could be relevant to the correlation between Parkinson's disease and melanoma,” added Lee.
To find out whether Pmel and α-synuclein have the ability to interact, the team utilized western blotting and microscopy to demonstrate that both proteins are present in the melanosomes of human melanoma cells.
In a test tube comprising the amyloid-forming area of Pmel (called the repeat, or RPT, domain), Dean introduced preformed α-synuclein amyloid and observed that the α-synuclein fibrils activated Pmel to clump and create a twisted structure of fibrils. The protein does not usually adopt this fibril structure on its own.
Since α-synuclein in melanoma cells may also exist in its non-amyloid, or soluble form, the investigators conducted more in vitro experiments where they introduced soluble α-synuclein to the Pmel RPT domain.
In this example, α-synuclein blocked the ability of Pmel to self-aggregate and create amyloid in a concentration-dependent way. The researchers followed this activity to the first 60 amino acids of α-synuclein.
We now have preliminary data that suggest an amyloid from one protein can 'seed' or template amyloid from another, and in the soluble form, α-synuclein prevents Pmel aggregation.”
Jennifer Lee, PhD, Postdoctoral Advisor, National Heart, Lung, and Blood Institute
“Therefore, we think that both forms of α-synuclein could diminish melanin biosynthesis -- the amyloid form by causing Pmel to form an unusual twisted structure, and the soluble form by stopping Pmel from aggregating like it should,” added Lee.
According to the researchers, loss of skin pigmentation may contribute to an increased risk of melanoma in patients with Parkinson's disease.
“I think we’re just at the tip of the iceberg of appreciating what α-synuclein might be doing in melanoma. In future experiments, I’m really interested in understanding more about what α-synuclein is doing to promote melanoma proliferation, in addition to this interaction with Pmel,” Dean concluded.