An international team of researchers has explained the action mechanism of incretin-based medications in diabetes treatment.
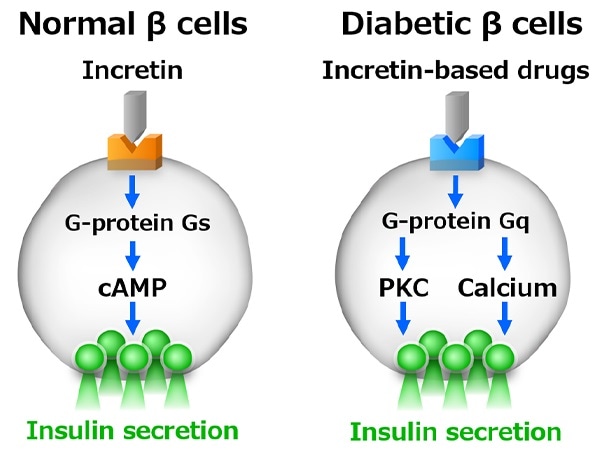
cAMP (cyclic AMP): An intracellular signaling molecule that regulates a variety of cellular functions such as insulin secretion. PKC (Protein Kinase C): An enzyme that adds phosphoric acid to proteins (phosphorylation), thereby regulating various intracellular signals such as insulin secretion. Image Credit: Kobe University.
The researchers, led by Professor SEINO Susumu, involved Researcher Okechi Oduori et al. from the Division of Molecular and Metabolic Medicine at Graduate School of Medicine in Kobe University; Professor SHIMOMURA Kenju from Fukushima Medical University, Professor Patrik Rorsman from the University of Oxford, the United Kingdom/the University of Gothenburg, Sweden), and their groups.
Incretin-based drugs are utilized globally for treating diabetes, and in Japan, these medications are presently prescribed to 70% of patients with diabetes. But the mechanism through which incretin-based drugs enhance blood glucose levels has not been clearly interpreted.
The study results were published online in the Journal of Clinical Investigation—the American Scientific Journal—on November 16th, 2020. A commentary on this article by Professor Colin G. Nichols and his collaborators from Washington University, St Louis, has also been published.
Main point
For the first time, the study has demonstrated that Gs, a crucial G-protein signal found in normal pancreatic β-cells, is changed to Gq, another G-protein signal found in the diabetic β-cells, to stimulate the secretion of insulin, and that incretin-based drugs work on this Gq to stimulate the secretion of insulin, and thus enhance blood glucose levels.
Research findings
Incretins are actually the gut hormones that are released by enteroendocrine cells following the ingestion of meals. The most significant function of incretins is to support the secretion of insulin from pancreatic β cells. GIP and GLP-1 are called incretins.
Although both GIP and GLP-1 are needed to sustain normal blood glucose levels in healthy individuals, incretins in type-2 diabetic (T2D) patients do not work properly. As such, incretin-based medications are mainly used for treating T2D to enhance the action of incretin. But the reason regarding the efficacy of these drugs has remained elusive.
The study examined the mechanism of insulin secretion by G-protein signaling in both diabetic β cells and normal β cells. So far, it has been well acknowledged that the G protein Gs works as an important signal that stimulates the secretion of insulin in normal β cells.
The researchers disclosed that in diabetes, there is a change from Gs to Gq signaling in the pancreatic β cells because of the continuous excitation of β cells. The team also found that incretin-based medications act on Gq signal to increase the secretion of insulin, thereby enhancing blood glucose levels.
The significance of this research
The study results are significant for elucidating the mechanism behind diabetes and also for diabetes treatments. They might also offer a groundwork for developing novel treatments.
Gs/Gq signaling switch in β cells underlies the potential of incretins in diabetes
Video Credit: Kobe University.
Source:
Journal reference:
Oduori, O. S., et al. (2020) Gs/Gq signaling switch in β cells defines incretin effectiveness in diabetes. Journal of Clinical Investigation. doi.org/10.1172/JCI140046.